Blog
-
Do You Have a Wart?
posted: Dec. 29, 2023.
Warts on the feet are a very common problem. The wart is caused by a virus that can be found just about anywhere. If you have a small scratch or Read more -
Common Foot Problems: Exploring Conditions Treated by Podiatrists
posted: Dec. 28, 2023.
-
Diabetic Foot Care: Preventing Complications and Maintaining Foot Health
posted: Dec. 09, 2023.
-
Forefoot Pain & Freiberg's Disease
posted: Dec. 07, 2023.
What is Freiberg’s Disease? This is a condition that is characterized by cartilage degeneration of the lesser metatarsal heads. This often leads to infarction and fracture of the metatarsal heads.Most commonly Read more -
Preventing Foot Injuries: Tips for Proper Foot Care and Injury Avoidance
posted: Dec. 01, 2023.

-
The Benefits of Seeing a Podiatrist
posted: Nov. 07, 2023.

-
The Benefits Of Orthotics
posted: Nov. 01, 2023.

-
Are you worried about lumps or bumps on your feet?
posted: Oct. 19, 2023.
Bumps can manifest as a wide variety of different pathologies. Usually depending on where they are in the Read more -
When To See a Podiatrist
posted: Oct. 06, 2023.

-
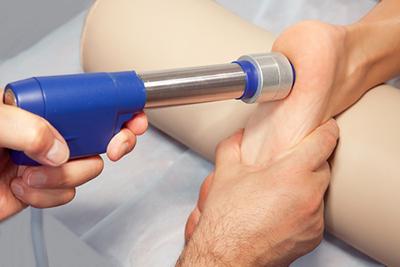
What Is Shockwave Therapy (EPAT) and How Does It Work?
posted: Oct. 04, 2023.
-
The Importance of Diabetic Care
posted: Oct. 01, 2023.

-
Let's Talk About Plantar Fasciitis...
posted: Sep. 26, 2023.
What is Plantar Fasciitis? “itis” is the medical term for “inflammation,” or inflammation of the plantar fascia. The plantar fascia is a ligamentous-like Read more -
Treating Your Bunion Symptoms
posted: Sep. 15, 2023.

-
Bunion Treatment Options
posted: Sep. 01, 2023.

-
Tips for Managing Your Arthritis:
posted: Aug. 28, 2023.
Thousands of Americans suffer from Arthritis daily. This can vary from a very mild condition to extremely limiting and disabling. Joint pain Read more -
Does Your Big Toe Joint Crack and Snap when you move it?
posted: Aug. 24, 2023.
Healthy joints are pain free joints. If you have been in an accident or dropped something heavy on your foot in the area of your big toe joint, you may Read more
Contact Us
Send Us an Email
Our Locations
Find us on the map
Hours of Operation
Our Regular Schedule
Prosper Office
Monday:
8:00 am-12:00 pm
1:00 pm-5:00 pm
Tuesday:
8:00 am-11:30 am
1:30 pm-5:00 pm
Wednesday:
8:00 am-1:00 pm
1:30 pm-5:00 pm
Thursday:
8:00 am-12:00 pm
1:30 pm-6:30 pm
Friday:
8:00 am-12:00 pm
1:00 pm-3:30 pm
Saturday:
Closed
Sunday:
Closed
McKinney Office
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
9:00 am-6:30 pm
Thursday:
8:00 am-5:00 pm
Friday:
7:30 am-4:00 pm
Saturday:
Closed
Sunday:
Closed
