Blog
-
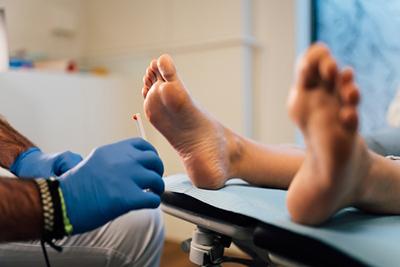
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 08, 2024.

-
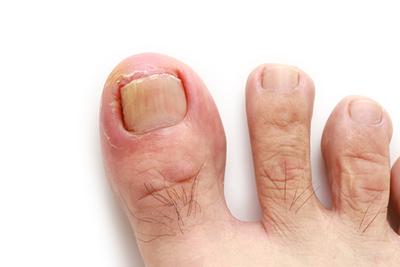
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
-
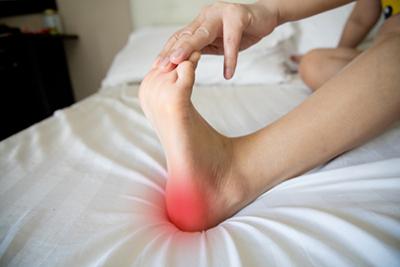
When To Seek Medical Help for Heel Pain
posted: Mar. 27, 2024.
-
Treating Plantar Fasciitis
posted: Mar. 15, 2024.
-
Lumps and Bumps
posted: Mar. 04, 2024.
Soft tissue masses to the top or side of your foot or ankle is a common concern for patients that visit our practice. These lumps usually start off small and Read more -
Achilles Tendonitis and How to Treat it
posted: Mar. 04, 2024.
The Achilles tendon is the largest and strongest tendon in the body, located in the back of the lower leg and connecting the heel bone to the calf muscle. This Read more -
Managing Your Heel Pain
posted: Mar. 01, 2024.
-
The Role of Podiatry in Managing Foot and Ankle Fractures
posted: Feb. 12, 2024.
-
What You Need To Know About Ingrown Toenails
posted: Feb. 01, 2024.
-
Do you roll or sprain your ankle often? Did you recently experience a bad rolled ankle? Options for ankle sprains and instability
posted: Jan. 19, 2024.
Could your ankle weakness be due to ankle instability? If so, find out how to address this problem. Have you experienced ankle injuries in the past? Were you someone who just Read more -
Big Toe Joint Arthritis
posted: Jan. 19, 2024.
Big Toe Joint Arthritis (Hallux Limitus/Rigidus) Arthritis in the big toe joint can be very painful and debilitating. This joint is very important for a proper walking pattern, and when it Read more -
Ankle Arthritis
posted: Jan. 19, 2024.
Arthritis is a common ailment that millions suffer from in the United States and around the world. The most common form is osteoarthritis which is caused by the Read more -
Chronic Ankle Pain and Ankle Arthroscopy
posted: Jan. 19, 2024.
Do you suffer from chronic ankle pain? Ankle arthroscopy may be the answer for you! Ankle arthroscopy is a minimally invasive procedure that helps to clean out the tissues and fluid Read more -
Do Your Toes Do Weird Things When You Walk? The Facts About In-Toeing and Toe-Walking
posted: Jan. 19, 2024.
Toe Walking and Intoeing: the Facts A very common question is whether kids who walk on their toes or walk intoed will “grow out of it”. In truth it is a Read more -
Sports Podiatry: Addressing Foot and Ankle Injuries in Athletes
posted: Jan. 08, 2024.

-
Orthotics and Their Role in Foot Health: Custom Solutions for Various Conditions
posted: Jan. 01, 2024.

Contact Us
Send Us an Email
Our Locations
Find us on the map
Hours of Operation
Our Regular Schedule
Prosper Office
Monday:
8:00 am-12:00 pm
1:00 pm-5:00 pm
Tuesday:
8:00 am-11:30 am
1:30 pm-5:00 pm
Wednesday:
8:00 am-1:00 pm
1:30 pm-5:00 pm
Thursday:
8:00 am-12:00 pm
1:30 pm-6:30 pm
Friday:
8:00 am-12:00 pm
1:00 pm-3:30 pm
Saturday:
Closed
Sunday:
Closed
McKinney Office
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
9:00 am-6:30 pm
Thursday:
8:00 am-5:00 pm
Friday:
7:30 am-4:00 pm
Saturday:
Closed
Sunday:
Closed